|
I was diagnosed with prostate cancer at a relatively young age of 55 last year. It was a shock to me as I had no symptoms and was in excellent health.
The biopsy revealed a Gleason 7 at stage T1C which basically means a moderately aggressive tumour that is still well contained within the prostate. Now there is a lot of confusion and noise out there about prostate screening and whether it unveils too many false-positives and that most men die “with” prostate cancer not “of” prostate cancer. The media is filled with stories such as Most Men Don’t Need a PSA Test that mainly came from a position by the US Preventative Services Task Force. In 2012, the task force recommended that doctors stop PSA screening of all men because many more men “will experience the harms of screening and treatment of screen-detected disease than will experience the benefit.” Well I just wanted to say that most urologists I have spoken to disagree with this opinion. While it is true that some older men with lower Gleason scores may not need to do anything, in my case it saved my life! My family doctor noticed in rise in my PSA. By having it checked periodically I had a baseline for him to provide an opinion. The sudden rise suggested he should refer me to a urologist. After many types of non-invasive testing my new urologist was adamant that I have a biopsy. My DRE (Digital Rectal Exam) was normal. My PSA was around 4.5 which is not HUGE. I went anyway after much research. When I finally opted for surgery in November of 2015, the pathology confirmed a Gleason 7 tumor and upgraded the stage to T2C. That is the last stage before the cancer breaks out of the prostate and metastasizes, usually to the bones. It would have killed me. Roughly 4,100 men will die of the disease in Canada this year, making it the second deadliest cancer among American men, after lung cancer. Knowledge is power. Get checked!.
1 Comment
This is a tough one. I firmly believe that my screening allowed me to detect a medium-aggressive form of prostate cancer very early. So early that I was debating about doing anything. On the flip side, the smaller the cancer and the younger the man gives one better odds at not only side effects but also survival.
In discussing this issue with my peers at the Burnaby Prostate Group it seems treatment was doled out more indiscriminately years ago. I think doctors are more open to active surveillance now. It is still a tough choice to make. Dr. Eric Hyndman says “The concern with the PSA test is that it doesn’t necessarily discriminate between low- and high-grade disease. We don’t need to identify these low-grade diseases. We do need to identify these high-grade diseases.” He says men have about a one-in-six chance of being diagnosed with prostate cancer, but only a one in 30 chance of dying from it. However Dr. Hyndman goes on to say “It’s still the second-leading cause of cancer-related deaths in men,” Hyndman said. I went ahead with surgery after six months of research even though I had no symptoms. The final pathology? Gleason 7 a moderately aggressive form of prostate cancer. Read More In this blog Dr. Moore explains how he almost became an accountant until he developed mono. Then at university he changed direction to oncology after visiting patients at Princess Margaret Cancer Centre. He is now president of the BC Cancer Agency. Whenever I visited B.C., I was always impressed by the passion and commitment of the staff at BC Cancer Agency and the research centres. I was excited to join the Agency, as I did last fall, because of its model of a patient-centred and integrated cancer care and research system. It’s very unique, and I saw great potential. Being close to the patients has always been important to me. That’s why I was happy to return recently to clinical practice one day a week. I missed seeing patients and also feel that working in a clinical setting will give me a greater understanding of the challenges and opportunities. Read More In this article researchers are trying to find out what your chances of dying from prostate cancer are so that you can make a better choice on treatment. A radical prostatectomy could be avoided by some.....
Researchers at the University of Copenhagen have identified a new prognostic biomarker: the neuropeptide pro-NPY, which may help determine the risk of dying from prostate cancer. This particular type of protein is very specific to prostate cancer cells and could help identify whether newly diagnosed patients require radical prostatectomy surgery or if it is safe to delay surgery. Using mass spectrometry, the researchers measured concentration changes in thousands of proteins in both normal and tumour tissue from prostate cancer. They discovered that in comparison to normal tissue, the prostate tumors exhibit numerous metabolic alterations including exacerbated activity of mitochondria. Read More In this study men with lower risk prostate cancer were found to benefit from waiting and watching. I would imagine that would be Gleason 6 and lower. I would love to see a study on Gleason 7 patients as that is a more difficult decision.
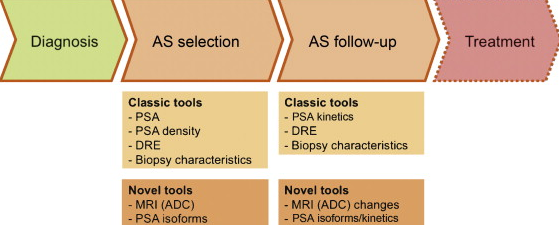
Is active surveillance a trustworthy and viable method to manage prostate cancer in a variety of practice settings — that is, outside the small group of academic centers that have pioneered and proven the approach in North America? The answer appears to be yes — in the short run at least, according to findings from a nine-site cohort study that includes a Veterans Administration (VA) hospital and a community-based practice. "Active surveillance is safe and a good initial strategy. About 10% to 15% of men fall off each year and transition to treatment," summarized investigator Daniel Lin, MD, a urologist at the University of Washington and Veterans Affairs Puget Sound Health Care System in Seattle. Read More Despite all the media controversy about PSA tests we all know that prostate cancer can be cured if caught early enough. The challenge for most men is that early prostate cancer has no symptoms but the side effects can seem severe enough to consider postponement of treatment. A graph of survival rates of patients given treatment compared with those who do not have it shows little difference in the first four years but after that, the survival rates for treated patients grows exponentially higher. If you are faced with this diagnosis give us a call at Prostate Cancer Burnaby Support Group Read more This is a very important article for those of us who have to make tough decisions very early on. This is often the case with early screening. Diagnosed with prostate cancer, we often leave the doctors office totally bewildered with a stack of flyers and a recommendation for treatment. "In the end it's your choice" we are told. We look at our PSA and Gleason scores as well as the potential side-effects of different treatment options. This PubMed article concludes that there are consistently higher mortality for patients treated with radiotherapy rather than surgery. Read the article here Scientists in France have found that fat cells may play a key role in how prostate cancer cells move. A team at the University of Toulouse found that, in mice, fat cells surrounding the prostate release a protein called CCL7, which sticks to a molecule on the surface of prostate cancer cells called CCR3. “The next step is to assess if this approach could benefit men with the disease.” - Dr Áine McCarthy, Cancer Research UK This interaction was able to help the cancerous cells move and spread in the mice, according to the study published in Nature Communications. By looking at tissue samples from men with prostate cancer, they also showed that higher levels of the CCR3 molecule were more common in more aggressive forms of the disease. And in tissue samples with higher levels of CCR3, the cancer cells were seen to move outside the prostate gland to the surrounding fat tissue. “This research in mice sheds light on why obese men with prostate cancer are more likely to have aggressive tumours,” said Dr Áine McCarthy, science information officer at Cancer Research UK. “It shows for the first time how fat cells surrounding the prostate use chemical signals to talk to tumour cells, enticing them to move and spread around the body. Excitingly, the researchers proved that jamming communications between fat cells and tumour cells stopped the cancer spreading. “The next step is to assess if this approach, using drugs that are already being developed, could benefit men with the disease,” she added. Read More "The electricity is so powerful they have to be paralysed while we're doing it or they would just jump off the table."
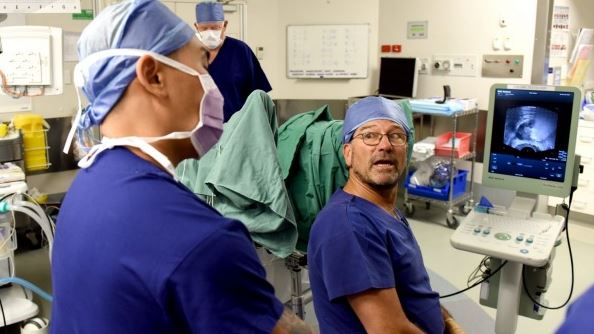
This was St Vincent's Private Hospital urologist Phillip Stricker, speaking of an emerging treatment for prostate cancer that involves zapping the tumour with more electricity than a bolt of lightning. Patient Rob Gunn, 65, was unconscious on the operating table, legs aloft, with four needles framing the site of the cancer. When the doctors switched on the machine, his legs began to jerk. Over the next 10 minutes, 90 pulses of electricity passed between the needles, exposing each centimetre of tissue to up to 1500 volts. By the end, the lesion had completely disappeared. "You can't underestimate the potential of this technology," Professor Stricker said. "It's going to save a lot of people from having unnecessary surgery." Read More It is the time of the year when no one can escape the traditional slew of diet and healthy lifestyle advice. Now any man seeking to shed the Christmas pounds may have an extra reason to get on that treadmill as a new study will examine how exercise affects prostate cancer survival. A group of men already suffering from the illness will undergo weekly aerobic sessions by researchers to explore the possible health benefits. Backed by Cancer Research UK, it is hoped the year-long study will lead to a full trial, thought to be the first of its kind. Read More |
AuthorThis blog is put together by a member of the Prostate Cancer Burnaby Support Group. Archives
July 2016
Categories |





 RSS Feed
RSS Feed